- Home
- About Us
- Why BFI
- Treatments
Advanced IVF Treatment
Donor Services
Fertility Preservation
Advanced IVF Treatment
Donor Services
Fertility Preservation
- Locations
- Resources
- Contact Us
Endoscopy Operations
Endoscopy is the direct observation of the inside of an organ or a cavity through an endoscope (telescope).
An endoscope is a tube with illumination connected to a high-resolution medical-grade video camera, monitor and recording system.
Laparoscopy to look inside the abdomen and Hysteroscopy to look inside the uterus are the most common modes of endoscopy used in infertility and gynaecology.
The advantage is that it is minimal access, so it has minimal or no cuts or scars. Practically all major or minor surgical procedures related to infertility and gynaecology can be done by Laparo-hysteroscopy.
If required in a patient, we at BFI perform both Hysteroscopy and laparoscopy at the same sitting to save time, cost and suffering.
Hysteroscopy
‘Hystero’ means uterus, and ‘scopy’ means to look; looking inside the uterus with the help of an endoscope is called Hysteroscopy.
Hysteroscopy can be done to diagnose any problem – diagnostic Hysteroscopy or correct any abnormalities in the uterus – operative hysteroscopy.
BFI has the policy of doing diagnostic and operative Hysteroscopy at the same sitting. We are always prepared to treat any unexpected problem detected. Patients have the advantage of saving a second operation, time and money.
A routine pre-IVF hysteroscopy is recommended in many cases to rule out any problem inside the uterus that may interfere with the implantation of embryos (embryo sticking) or the successful progress of the pregnancy. Correction of even minor problems or defects can substantially improve the IVF treatment outcome.
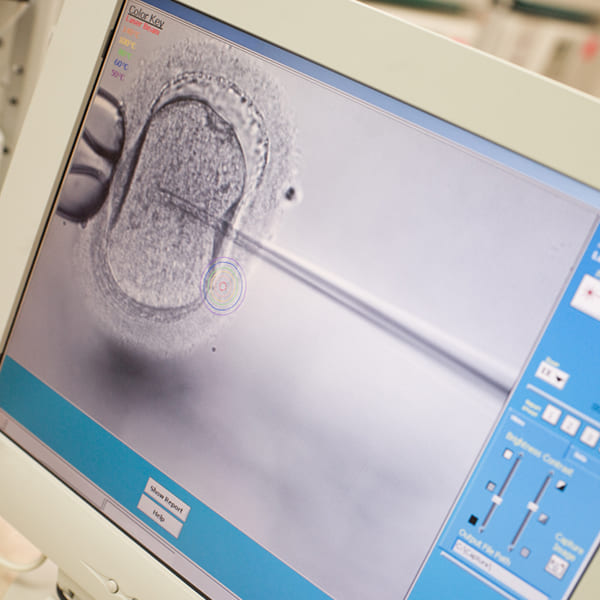
In women facing repeated miscarriages, Hysteroscopy can be an invaluable tool to diagnose the cause or treat any defect or problems.
Even when there are normal hysteroscopy findings, endometrial activation, endometrial scratch, cavity enhancement, uterine cavity wash etc., can improve the outcome of subsequent treatment cycles.
According to the general consensus amongst world fertility specialists, Hysteroscopy is a necessary part of the investigation and treatment of IVF failure. In our own experience, many patients of repeated IVF or Implantation failure have got successful live birth in the treatment cycles following Hysteroscopy.
What can be treated successfully with Hysteroscopy
Shape abnormalities
Septum – A partial or complete division of the uterus by a curtain-like structure. “T” shaped uterus is a narrow and less developed uterine cavity.
Narrow cervix – cervical stenosis
Other problems affecting fertility
- Adhesions in the uterus,
- Asherman’s syndrome- dense adhesions in the uterus
- Fibroid removal for fibroid that is in the uterine cavity – Submucous fibroid
- Polyp removal
- Uterine septum correction
- Removal of retained bits of foetal and placental tissues or bones after miscarriage
- Tube opening procedure – tubal/ cornual cannulation for opening the blocked fallopian tubes.
Other uses for diseases of women
- Misplaced IUCD/ copper T removal
- Any foreign body removal
- Biopsy to diagnose cancer or other problems
- Remove endometrium to cure excessive bleeding problems TCRE
How is Hysteroscopy done?
Hysteroscopy is a procedure done under mild anaesthesia. The typical duration of the procedure is 10-20 minutes as the scope is introduced through the cervix (mouth of the uterus). There is no cut or scar.
Simple diagnostic and operative Hysteroscopy are very safe with very little chance of major complications.
BFI uses a very advanced 1.9 MM and 2.9 MM Hysteroscopy set up for minimum manipulations and an extremely safe bipolar resectoscope. We do most of our procedures with scissors only to avoid any excessive exposure and possible damage to the most precious and sensitive endometrium.
Complete visualization and examination of the whole uterine cavity are done. Any problem diagnosed is corrected at the same time. All the findings are photographed and video recorded and given to the patients for records and future reference.
Usually, a patient can take fluid and then food after 2 hours of the procedure and can go home.

What are the risks?
For prolonged procedures, the fluid used to expand the uterine cavity can cause fluid overload and related issues.
At BFI, we use special automatic pressure monitored “hysteroflater” to minimize the risk of this complication.
Damage to endometrium
We use scissors for most of our surgeries, as far as possible. We use a bipolar resectoscope and use minimum current.
Infection, anaesthesia related complications and other complications are very uncommon or rare.
Advantage hysteroscopy
- No scars
- No long hospital stay
- Minimum anaesthesia and manipulations
- Practically ALL problems inside the uterus can be treated
Disadvantage hysteroscopy
- Requires a very expensive high tech set up for optimal results
- Requires skills and experienced surgeon for optimum results
Laparoscopy

‘Laparo’ means abdomen, and ‘scopy’ means to look; looking inside the abdomen with the help of an endoscope is called laparoscopy. Laparoscopy provides clear visualization of organs inside the abdomen like the uterus, tubes, ovaries and surrounding structures.
What can be treated successfully with laparoscopy
Practically all the operations for diseases of women which required a big cut on tummy – Laparotomy – can now be done with minimum access surgery – minimum invasive surgery – laparoscopy.
For fertility treatment
- Diagnostic laparoscopy for diagnosis of any problem
- Drilling of Poly Cystic Ovaries – PCO drilling – Laparoscopic ovarian diathermy – LOD
- Endometriosis
- Mild – moderate-severe – rectovaginal
- Cysts in the ovary
- Chocolate Cyst – endometrioma of the ovary
- Dermoid Cyst
- Other Cysts
- Fibroids
- Small fibroids – Big fibroids – Multiple fibroids
- Intra mural fibroid– subserous fibroid – broad ligament fibroid
- Ectopic Pregnancy management – conservative – Tube saving
- Tube removal – salpingectomy
- The fallopian tube opening surgery – Tubectomy reversal opening the tubes after tubal ligation (family planning operation)
Block tube opening surgery – Salpingostomy
- Adhesions removal – Adhesiolysis
- Tuboovarian Mass removal
- Ovarian rejuvenation
- Ovarian transplantation
- Creation of vagina – Vaginoplasty
- Correction of the divided uterus – unification operation for bicornuate uterus
Other than fertility – general gynaecology – diseases of women
- Hysterectomy – Total or Subtotal – TLH Total laparoscopic hysterectomy
- Ovarian cyst removal – Cysts of the ovary
- Fibroids
- Endometriosis
- Adhesiolysis – TO mass removal – presacral neurectomy
- Vaginoplasty
- Vault prolapse surgery
- Os tightening – Laparoscopic cervical cerclage
- Tubal Ligation (for family planning)
- Uterus Prolapse Repair with Preserving Uterus
- Vesico vaginal fistula repair VVF repair
- Repair of perforation of the uterus
- Remove misplaced IUCD – Cu T
- Removal of the rudimentary horn of the uterus
How is laparoscopy done?
Laparoscopy is performed under general anaesthesia. A needle is inserted through the navel to fill the abdominal cavity with carbon dioxide gas. The gas moves the abdominal wall away from the wall of the internal organs so that the laparoscope can be safely placed in the abdominal cavity.
Whether the tubes are open or not is checked by injected a blue die from the uterus. The die flows through the tubes and can be seen entering the abdomen from the tubes when the tubes are open. In case of finding any alteration, we can intervene at that very moment and thus try to solve it.
Depending upon the nature and complexity of the surgery, a number of instruments are used. Most instruments are only pencil size; thus, the small cuts may not require stich also. After completion of the operation, a thorough check for bleeding is done, abdomen cavity is washed, CO2 gas removed completely, instrument count checked stitches taken if needed, and then the patient is brought back to consciousness.
BFI has a high-resolution medical camera and a whole endoscopy system that enables us to use 5 mm telescopes and 3 MM instruments for most of our surgeries. Minimal invasive becomes least invasive!

What are the risks?
It requires operation inside the abdomen, so damage to other vital organs can rarely occur.
It requires full anaesthesia, so problems related to prolonged anaesthesia can occur.
Excessive blood loss, infection, thromboembolism are uncommon or rare complications.
Advantage laparoscopy
- Very small scars
- Very fast recovery
- Minimum chances of adhesion formation
- Minimum post-operative pain
- No long hospital stay
- Minimum manipulation of internal organs
- Practically ALL women’s problems requiring surgery in the abdomen can be treated
Disadvantage hysteroscopy
- Requires a very expensive high tech set up for optimal results
- Requires skills and experienced surgeon and team for optimum results
- Expensive disposables and consumables
Cutting edge technology for effective & safer endoscopy
Lapro-hysteroscopy is a technically advanced procedure. If proper technique is not used, results may not be optimum or sometimes complications due to surgery may be more. We use this cutting edge technology for safer endoscopy.
- HD endoscopy to get the clearest vision
- All scope sizes from office hysteroscopy to scope for major surgeries to ensure minimal invasive surgery, always including office hysteroscopy.
- Hysteroflator for preventing any fluid overload complications in Hysteroscopy
- Vessel sealing device
- Underwater bipolar cautery for safe hysteroscopic fibroid and other surgeries
- Specialized anaesthesia workstation for minimum use of anaesthetic gases for faster post-operative recovery
- CO2 gas monitoring by ETCO2 for safe anaesthesia
- Specialized video recording, documentation and reporting software
Note: Exact instrument may vary for different centres
BFI takes pride in doing a wide variety of most complicated and difficult surgeries successfully!



